NIH-funded study provides evidence on transplantation practice currently limited to research settings.
October 17, 2024 – Kidney transplantation from deceased donors with HIV (HIV D+) to recipients with HIV (HIV R+) was safe and comparable to kidney transplantation from donors without HIV (HIV D-) in a multicenter observational study in the United States. The clinical outcomes observed were consistent with smaller pilot studies, but this National Institutes of Health (NIH)-funded clinical trial was the first statistically powered to demonstrate noninferiority, which 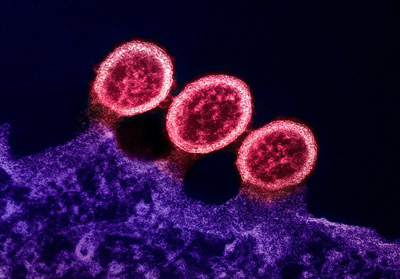 means that an approach being studied is as good as standard clinical practice. The results were published today in the New England Journal of Medicine.
means that an approach being studied is as good as standard clinical practice. The results were published today in the New England Journal of Medicine.
(Pictured) Transmission electron micrograph of HIV-1 virus particles.
Kidney transplants offer a survival benefit to people with HIV and end-stage kidney disease, but an organ shortage limits access. In addition, people with HIV face a higher risk of death while on the organ waitlist and have lower access to transplants than people without HIV. To help address these disparities, the HIV Organ Policy Equity Act (HOPE) was implemented in 2015 and legalized transplants between donors and recipients with HIV. Currently, the HOPE Act limits this practice to research settings to carefully evaluate outcomes. These include post-transplant survival, post-transplant kidney function (also known as graft survival), and kidney rejection. Research studies also assess unique potential risks of this practice, such as acquiring a second, genetically distinct HIV strain from the donor that could affect the recipient’s HIV disease.
The present study enrolled 198 adults with HIV and end-stage kidney disease who received kidney transplants at 26 centers, comparing the outcomes of 99 study participants who had donors with HIV versus 99 whose donors did not have HIV. Transplants were completed between April 2018 and September 2021 and recipients were monitored subsequently for about three years.
The outcomes for overall survival, graft survival, and rejection events were similar between the two groups. After one year post-transplant, recipient survival was 94% in HIV D+/R+ and 95% in HIV D-/R+. At three years, recipient survival rates were 85% in HIV D+/R+ and 87% in HIV D-/R+. After one year post-transplant, graft survival was 93% in HIV D+/R+ and 90% HIV D-/R+. At three years post-transplant, graft survival rates were 84% in HIV D+/R+ and 80% in HIV D-/R+. Finally, at one year post-transplant, rejection incidence was 13% in HIV D+/R+ and 21% HIV D-/R+ and at three years, 13% in HIV D+/R+ versus 21% in HIV D-/R+. Rates of serious adverse events, surgical site infections, surgical/vascular complications, and cancer were also comparable between the two groups. One case of a recipient who may have acquired a second genetically distinct HIV strain from their donor was observed, but there were no notable clinical consequences.
Overall, the findings show kidney transplantation between donors and recipients with HIV was safe and noninferior to transplantation from donors without HIV. According to the authors, these findings offer evidence to support the expansion of the practice outside of research settings.
The study was led by the Johns Hopkins University School of Medicine, Baltimore, and funded by NIH’s National Institute of Allergy and Infectious Diseases (NIAID).
For more information about this trial, please visit ClinicalTrials.gov using the study identifier NCT03500315.
ARTICLE: Durand et al. Safety of Kidney Transplantation from Donors with HIV under the HOPE Act. NEJM. DOI: 10.1056/NEJMoa2403733 (2024).
WHO: Andrew Redd, Ph.D., International Virology Unit, Head, Laboratory of Immunoregulation, National Institute of Allergy and Infectious Diseases.
NIAID conducts and supports research—at NIH, throughout the United States, and worldwide—to study the causes of infectious and immune-mediated diseases, and to develop better means of preventing, diagnosing and treating these illnesses. News releases, fact sheets and other NIAID-related materials are available on the NIAID website.
About the National Institutes of Health (NIH): NIH, the nation's medical research agency, includes 27 Institutes and Centers and is a component of the U.S. Department of Health and Human Services. NIH is the primary federal agency conducting and supporting basic, clinical, and translational medical research, and is investigating the causes, treatments, and cures for both common and rare diseases. For more information about NIH and its programs, visit www.nih.gov.
NIH…Turning Discovery Into Health®
Source & image: NIH








